What Are the Symptoms of Knee Bursitis?
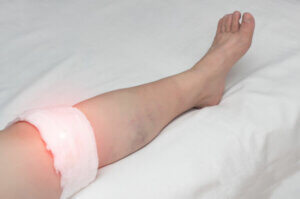
Just with any condition ending in “itis”, the main discomfort of bursitis is caused by inflammation. It can occur in various parts of the body wherever there’s a bursa. However, in this article, we’re going to focus on knee bursitis.
Bursa inflammation
Let’s start by explaining exactly what the bursa is. The small sacks of fluid around the knee joint are called bursas. Their job is to reduce friction and protect pressure points.
Why does it become inflamed?
There are several reasons why the bursas can become inflamed. These include overuse, injury, infection, exercising with a poor posture or repetitive movements.
Any of these can cause bursitis, and treatment will vary depending on the cause.
Symptoms of knee bursitis
As we’ve already mentioned, this is an “itis”, so the main symptom of knee bursitis is inflammation. This means that the affected area will swell, turn red, and become hotter, all because of the increase in blood supply.
As normally happens when there’s swelling, the movement will be limited. You might find it difficult to fully bend or straighten your leg and some movements might be painful.

Lastly, if the bursitis is caused by an infection, you may also have a fever.
Treatment for knee bursitis
Sometimes, bursitis will simply go away on its own. After a few days of inflammation, simply by resting, the area will recover and the swelling will go down.
However, it’s possible that you’ll have to take active steps to recover. This way, you can stop the symptoms getting worse and becoming chronic, as it can become a really annoying and limiting condition.
Rest
The first thing to consider is your rest. This means trying to use the joint as little as possible so that the bursa isn’t forced to cushion any weight.
Rest will be important anyway if bursitis has appeared because of an external injury so that both injuries can heal at the same time.
Elevation, ice, and compression
Along with rest, the first way to treat any inflammation is elevation, ice, and compression. Elevating the affected area means that gravity helps to drain the area. Meanwhile, ice reduces blood supply and compression encourages blood return.
Anti-inflammatories
Although it’s not a good idea to take them frequently, you might need anti-inflammatories. If you notice that your bursitis isn’t going away, a doctor may prescribe it for you to speed up recovery.
Physiotherapy
Going to a physiotherapist can also be a great help when recovering from knee bursitis. They’ll be able to use stretches, exercises, and other techniques to guide you towards recovery.

Injections for knee bursitis
If the condition seems to be becoming chronic, your doctor may recommend an injection of corticosteroids. This method is more aggressive and invasive, but it can help if necessary.
Antibiotics
Lastly, if bursitis has appeared because of an infection, your doctor may prescribe antibiotics. In this situation, you may also need to have the accumulated fluid drained in order to reduce the presence of the infection.
Just with any condition ending in “itis”, the main discomfort of bursitis is caused by inflammation. It can occur in various parts of the body wherever there’s a bursa. However, in this article, we’re going to focus on knee bursitis.
Bursa inflammation
Let’s start by explaining exactly what the bursa is. The small sacks of fluid around the knee joint are called bursas. Their job is to reduce friction and protect pressure points.
Why does it become inflamed?
There are several reasons why the bursas can become inflamed. These include overuse, injury, infection, exercising with a poor posture or repetitive movements.
Any of these can cause bursitis, and treatment will vary depending on the cause.
Symptoms of knee bursitis
As we’ve already mentioned, this is an “itis”, so the main symptom of knee bursitis is inflammation. This means that the affected area will swell, turn red, and become hotter, all because of the increase in blood supply.
As normally happens when there’s swelling, the movement will be limited. You might find it difficult to fully bend or straighten your leg and some movements might be painful.

Lastly, if the bursitis is caused by an infection, you may also have a fever.
Treatment for knee bursitis
Sometimes, bursitis will simply go away on its own. After a few days of inflammation, simply by resting, the area will recover and the swelling will go down.
However, it’s possible that you’ll have to take active steps to recover. This way, you can stop the symptoms getting worse and becoming chronic, as it can become a really annoying and limiting condition.
Rest
The first thing to consider is your rest. This means trying to use the joint as little as possible so that the bursa isn’t forced to cushion any weight.
Rest will be important anyway if bursitis has appeared because of an external injury so that both injuries can heal at the same time.
Elevation, ice, and compression
Along with rest, the first way to treat any inflammation is elevation, ice, and compression. Elevating the affected area means that gravity helps to drain the area. Meanwhile, ice reduces blood supply and compression encourages blood return.
Anti-inflammatories
Although it’s not a good idea to take them frequently, you might need anti-inflammatories. If you notice that your bursitis isn’t going away, a doctor may prescribe it for you to speed up recovery.
Physiotherapy
Going to a physiotherapist can also be a great help when recovering from knee bursitis. They’ll be able to use stretches, exercises, and other techniques to guide you towards recovery.

Injections for knee bursitis
If the condition seems to be becoming chronic, your doctor may recommend an injection of corticosteroids. This method is more aggressive and invasive, but it can help if necessary.
Antibiotics
Lastly, if bursitis has appeared because of an infection, your doctor may prescribe antibiotics. In this situation, you may also need to have the accumulated fluid drained in order to reduce the presence of the infection.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Draghi, F., Corti, R., Urciuoli, L. et al. Knee bursitis: a sonographic evaluation. Journal of Ultrasound (2015) 18: 251. https://doi.org/10.1007/s40477-015-0168-z
- A. P. Le Manac’h, C. Ha, A. Descatha, E. Imbernon, Y. Roquelaure, Prevalence of knee bursitis in the workforce. Occupational Medicine, Volume 62, Issue 8, December 2012, Pages 658–660, https://doi.org/10.1093/occmed/kqs113
- Jensen, Lilli Kirkeskov, and Winnie Eenberg. Occupation as a Risk Factor for Knee Disorders. Scandinavian Journal of Work, Environment & Health, vol. 22, no. 3, 1996, pp. 165–175. JSTOR, www.jstor.org/stable/40966530
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.